I serve as director of spiritual care for a multi-hospital operating unit in a large urban health care system. A few months ago, as the nurse staffing shortage reached crisis level, our hospital leadership became concerned about the level of stress on nursing leaders. As part of the response, chaplains were asked to help facilitate “leader debrief meetings,” providing space for leaders to talk honestly as they tried to cope with the staff shortage and supply chain issues that impacted daily care management.
At my invitation, senior leaders attended these meetings and shared honestly from their own struggles to lead through the pandemic. In response, many mid-level leaders also opened up about how overwhelmed they felt trying to manage so much that was out of their control. I had a number of leaders express appreciation for these meetings and the opportunity to be vulnerable. They spoke of the need to hear from their colleagues going through similar challenges and to feel solidarity with each other.

Beth Jacson-Jordan
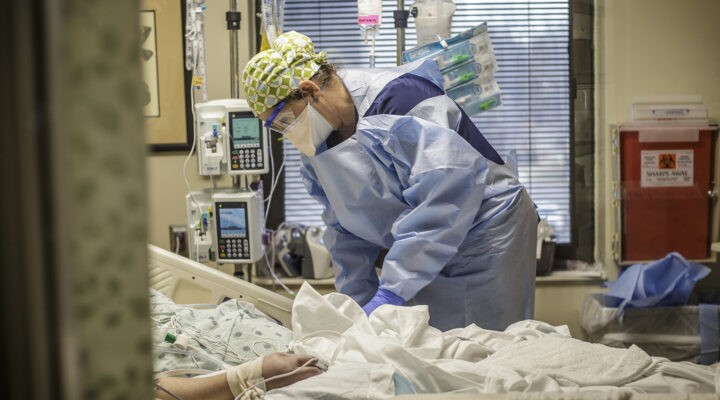
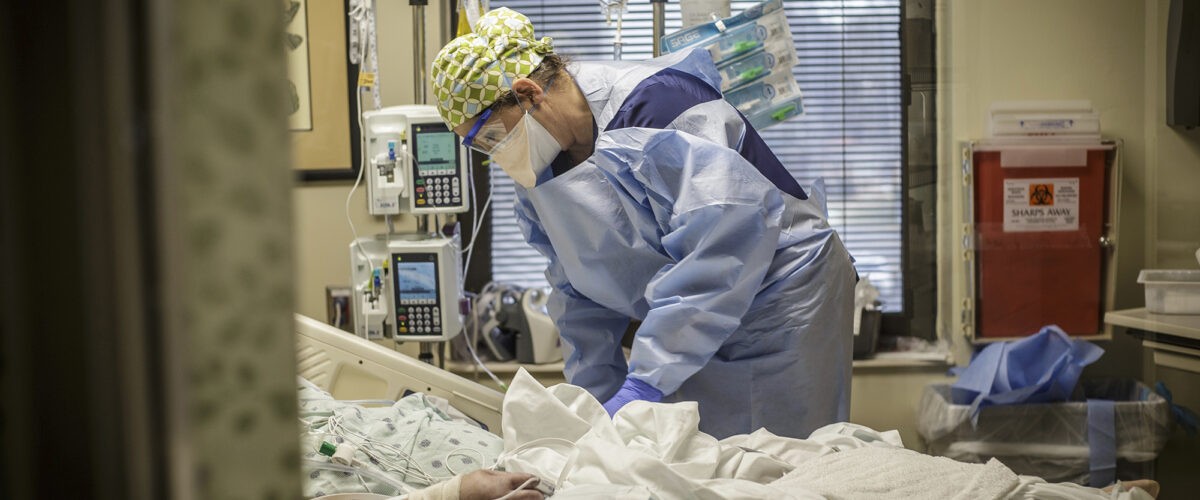
In the more than 30 years that I have served as a chaplain in various health care settings, supporting staff always has been a part of my role. To a large degree, that support has occurred informally by building relationships and checking in with staff especially during times of high stress or critical events. It also has included more structured forms of support such as leading memorial services, providing “Tea for the Soul;” events, offering the “Blessing of Hands” ritual and programs to teach resiliency skills.
Throughout the pandemic, the level of suffering borne by our staff became so critical that staff support became one of our greatest priorities as chaplains. We implemented additional support interventions and increased the amount of time spent rounding and checking in with all staff.
I believe our support as chaplains, along with the other sources of support provided by our health care system, had a positive impact. I’m also aware that the level of burnout and suffering for all staff in health care has reached a tipping point. People are leaving health care in record numbers. The pandemic has contributed greatly to the factors causing this exodus. However, I also believe the pandemic brought to light many systemic problems in health care that had made it increasingly problematic for those in direct caregiving roles.
A recent study by the American Medical Association found that one in five physicians and two in five nurses surveyed expected to leave their current practice within two years. One-third of both groups intended to reduce their hours over the next year.
The desire to leave the field of health care is being reported by all categories of workers. This is consistent with what I have witnessed in my own setting. In the past year, we have had growing numbers of resignations and early retirements of both front-line staff and leadership. Our number of temporary “traveling” nurses has increased significantly due to the number of resignations and difficulty filling those positions. This trend has impacted not only our nursing staff but all other departments — such as respiratory therapy, dietary, case management and the list goes on.
“As I’ve listened to staff and leaders in our hospital over the pandemic, it’s become clear to me that being applauded as heroes is not helpful.”
As I’ve listened to staff and leaders in our hospital over the pandemic, it’s become clear to me that being applauded as heroes is not helpful. The narrative of the sacrificial front-line worker allows us to ignore the human cost of our modern health care system. What our staff members need are reduced hours, better child care options, more paid time off and a workplace culture that prioritizes the emotional and physical well-being of staff. They need permission to talk about and address their mental health needs without fear of being viewed as weak. They need to have their challenges acknowledged and taken seriously.
I recently thought back on those leader-debrief meetings held several months ago and realized that many of those who attended, including some senior leaders, are gone. They are casualties of a health care system that not only was unprepared to manage a pandemic but also in denial of the unsustainable toll that modern health care takes on the staff who work in it.
The challenges of our current health care system are immense and will take monumental efforts to address. As a chaplain, I’m called to support the emotional and spiritual needs of our staff. I’m also called to tell the truth about our health care environment and the moral distress of those who serve in it.
This article originally was published by the Alliance of Baptists.
Beth Jackson-Jordan serves as director of spiritual health at the Emory DeKalb Operating Unit, which includes Emory Decatur, Emory Hillandale and Emory Long-term Acute Care Hospitals. She is ordained for ministry and endorsed to chaplaincy by the Alliance of Baptists. She is a board-certified chaplain with the Association of Professional Chaplains and is an ACPE Certified Educator.
Related articles:
This small book is for health care workers operating on a wing and a prayer
Me and my multicultural medical procedure | Opinion by Bob Newell
Through 14 months of pandemic, hospital chaplains have carried others’ burdens
How a Baptist educator and businessman’s simple plan gave rise to the health insurance industry