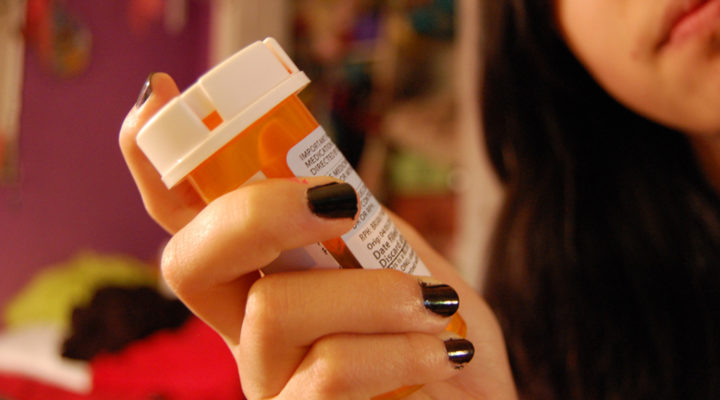
It begins with the pain. A 2011 study by the Institute of Medicine suggests that one in three Americans “suffer from chronic pain.” For Coloradan Melissa Morris the pain began after C-section childbirth. Her doctor prescribed Percocet, and even the first dose was transformative. “I remember thinking to myself,” she told NPR’s Luke Runyon, “‘Oh my god. Is this legal? How can this feel so good?’” Before long, she was hooked, moving from Percocet to Vicodin to injecting OxyContin. In the end, she turned to heroin, even “dealing” to fund her habit. Clean now, Morris’s experience mirrors the ever-expanding opioid epidemic sweeping America.
It begins with the pain. A 2011 study by the Institute of Medicine suggests that one in three Americans “suffer from chronic pain.” For Coloradan Melissa Morris the pain began after C-section childbirth. Her doctor prescribed Percocet, and even the first dose was transformative. “I remember thinking to myself,” she told NPR’s Luke Runyon, “‘Oh my god. Is this legal? How can this feel so good?’” Before long, she was hooked, moving from Percocet to Vicodin to injecting OxyContin. In the end, she turned to heroin, even “dealing” to fund her habit. Clean now, Morris’s experience mirrors the ever-expanding opioid epidemic sweeping America.
An April 2017 essay in Vox reports that 2015 brought the largest recorded number of deaths by drug overdoses ever recorded, over 52,000 in 12 months, some 33,000 of which related to opioids. Those figures outpaced casualties from car wrecks and gun violence, and at the height of the HIV/AIDS crisis in 1995 (43,000).
Opioids cut the pain, but only for the short-term, in drugs like OxyContin and Percocet, prescribed by physicians across the country. Extended consumption, however, opens the door to addiction. When the prescriptions run out, the resulting addicts often gravitate toward heroin, fentanyl, and the black market.
Others simply experiment, with dire results. A June 10 New York Times essay calls Internet sales of fentanyl the “fastest growing cause of national overdoses.” This “dark web” contributed to the 2016 deaths of two 13-year-olds from Park City, Utah, who overdosed on Pinky (U-47700), a synthetic opioid bought from a fellow teen who got it online.
The crisis is nationwide, but with varying regional intensity. Top 10 opioid-plagued states include West Virginia (at 35.5 cases per 100,000, the nation’s highest rate), New Mexico, New Hampshire, Kentucky, Ohio, Rhode Island, Utah, Pennsylvania, Delaware and Oklahoma. In 2016 Congress passed the Comprehensive Addiction and Recovery Act, aimed at expanding resources for medical professionals in assisting addicts. Potential changes in health care may significantly impact its continued implementation.
As the opioid crisis deepens, many churches are rising to the occasion. Last year, the West Virginia Council of Churches partnered with the state Department of Health and Human Resources to provide congregations with instruction in “screening, brief intervention and referral to treatment” (SBIRT). The Massachusetts Council of Churches also provides such guidance. Director Laura Everett reports: “We are overwhelmed by the demand of spiritual caregivers and interfaith colleagues who are reaching out to us to provide more training sessions. We really think that clergy can model a supportive, pastorally appropriate, nonjudgmental way of speaking about addiction in ways that break the stigma and isolation that often comes with addiction.” Some estimates suggest that five Massachusetts citizens die daily from substance abuse.
In an April 2017 article from Our Sunday Visitor, Father John Mahoney, director of clinical services for New Hampshire Catholic Charities, comments: “We noticed that addicted individuals were not coming to us for direct-care services. There is so much shame and guilt associated with substance use disorder, and individuals would be embarrassed to come to the Catholic Church for help.” Mahoney insists that the Church must respond to the opioid epidemic as a public health problem, treating drug abuse as a disease, not a sin. “Jesus didn’t stay in a clinic or in an office,” Mahoney adds, he “went to the marketplace and healed the people he met there.” Opioids carry faith communions into new ministries, often in neglected segments of society.
Janice Ford, Episcopal rector at the Church of the Reconciliation in Webster, Mass., agrees. A CommonHealth article cites her insistence that: “We’re not looking to convert folks. That’s not what this is about. When you provide spiritual care, you’re trying to find where is God in their addiction? Where is God in their life? That’s what lived spirituality means.”
Substance abuse is a complex issue because pain is multilayered, taking on parallel and distinct configurations in every human being. Questions abound: Are American churches up to the task of addressing opioid use in their communities and among their members? Can churches create task force responders who are trained enough to engage with families where addicts are present, offering compassion, counseling, and referrals? Are there indeed spiritual resources that can aid those for whom pain is real and guilt is deep? Can persons enmeshed in pain and Percocet feel safe enough in our congregations to seek physical, mental, and yes, spiritual assistance? Might American Christians, now so divided by doctrine, culture wars, and politics, find increasing new ways to work together in response to an epidemic impacting their neighbors inside and outside the church?
Reverend Ford captures the passion and the imperative of the moment: “Addiction is a disease. It’s not about people’s morals. Helping these people is the same as our efforts for Syrian refugees — although many people might not think of it like that. What each clergy person does depends on a few things: time, skills and passion. For me, this has taken over my life.”
Grace that is not present in the pain that haunts us every one, and the means we use to escape it, is no grace at all.
Related opinion:
Opioid abuse is a tragedy, crack cocaine use is a crime. Why? | Russ Dean