As many look toward local and state health departments, health care providers or even the news for trusted coronavirus information, people of faith are also leaning on faith community nurses.
A lesser-known specialty practice, faith community nursing aims to care for the body, mind and soul of members of congregations.
“We’re probably the best-kept secret around,” said Linda Garner, a faith community nurse at Wilshire Baptist Church in Dallas. Still, the Westberg Institute for Faith Community Nursing estimates there are 15,000 to 18,000 faith community nurses worldwide.
A nurses’ responsibilities can vary from phone triage to consoling someone whose parent passed away. And during the COVID-19 pandemic, that range has widened, making their hidden roles all the more major. That’s because, the nurses explain, people see them as trusted, reliable figures in a public health crisis rife with confusion and anxiety.
Both medical and spiritual
Faith community nurses have “one foot in the medical and one foot in the spiritual,” said Sharon Hinton, director of the Westberg Institute, the primary resource center for faith community nurses. “Nurses are experts in their field, and if you give them additional training on spiritual care as well, then they can take care of the whole person.”
“Nurses are experts in their field, and if you give them additional training on spiritual care as well, then they can take care of the whole person.”
Through the Westberg Institute, nurses may receive training from 100 assorted educational partners. They also may connect with two membership organizations, the Health Ministries Association and Faith Community Nurses International.
A nurse obtains the specialty license from the American Nurses Association after 30 hours of training in spiritual and emotional care, among other areas, Hinton said. The majority of faith community nurses volunteer with specific congregations, although others are employees of hospitals or health care systems. A Lutheran minister, Granger Westberg, founded the practice, but today, nurses serve in Jewish and Muslim communities in addition to Christian ones.
Before COVID-19, faith community nurses’ responsibilities included organizing flu shot clinics or blood drives, testing peoples’ blood pressure, loaning out church-owned walkers, using an AED, taking people to medical appoints and educating people about health concerns. Many times, congregants individually would reach out to nurses with medical questions.
New roles during pandemic
With the pandemic, nurses haven’t set aside their previous roles; they have adopted new roles as well.

Linda Garner
Garner, for example, serves on Wilshire’s COVID-19 task force to advise leadership on what kind of gatherings should be allowed and under what conditions. She’s also writing articles about health safety measures that go in two weekly church publications. Other times, she’s giving one-on-one advice, such as explaining the difference between quarantine and self-isolation, for example.
“People know me, they know that I am part of the staff. As such, they know they can rely on what I tell them,” said Garner, who also sits on the board of Faith Community Nurses International.
Other faith community nurses have been offering emotional care during the pandemic.
Marilyn Harris, a nurse at Hatboro Baptist Church in Pennsylvania, oversees the church’s congregational care ministry. As part of that, she helps run Hatboro’s bereavement ministry, a 13-month program that offers support to church members who have lost loved ones. There’s been more participation in the program this past year due to members dying from COVID-19.
Meanwhile, Harris has kept in contact with older church members who have been living in isolation. A few people have told her it feels like they are “being remembered and not lost in the shuffle,” Harris said. “People call me just to talk sometime. Which is great. I’m so happy that they are so comfortable.”

Susan Johnson
Susan Johnson, a program manager at Hoag Memorial Hospital Presbyterian in California, has observed a similar effort from faith community nurses who partner with Hoag. It’s common for faith community nurses to partner with larger, regional health care systems. Many nurses Hoag partners with serve churches with older congregants who also have been in isolation.
“It’s been really heartbreaking for the nurses because they want to be able to do more,” Johnson said. “They recognize that there is a lot of isolation and loneliness.”
In response, some nurses have visited peoples’ homes to talk by the front stoop. Others have even provided hospice care.
Vaccine education
Recently, faith community nurses have added another job to their repertoire: vaccine education. Garner, Harris and Johnson all described similar situations of congregants eligible to receive the COVID-19 vaccines being confused about where to sign up, and faith community nurses were able to point them in the right direction.
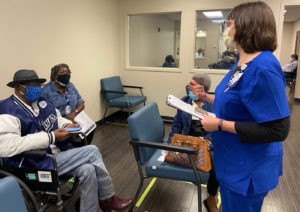
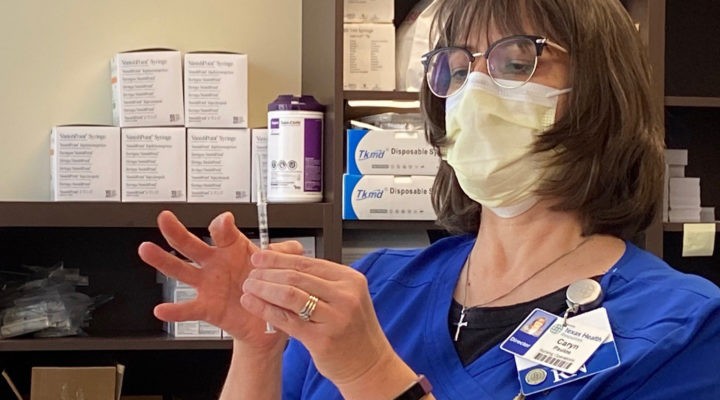
Caryn Paulos checks on patients who received the COVID-19 vaccine. (Photo courtesy of Texas Health Resources)
Caryn Paulos, director of the faith/community health improvement program at Texas Health Resources, one of the largest faith-based, nonprofit health systems in North Texas, described a similar, yet different phenomenon. It’s not just confusion about the vaccine that nurses in Texas Health’s network of 125 congregations are dealing with, it’s vaccine hesitancy.
Paulos said there’s been greater skepticism about the vaccine among predominantly Black and Hispanic congregations in Texas Health’s network, part of a nationwide trend. As a result, Paulos has been intentional about funneling information about the vaccine to nurses in those communities, who then relay it to congregants.
“It’s one thing for Texas Health to hand you information, but it’s another thing for nurses and faith leaders to say, ‘This information is accurate, I have looked through it, I understand it,’” Paulos said.
This approach has made a difference. One day, Texas Health, a vaccine distributor for the area, had extra doses. So, Paulos reached out to a nurse at a predominantly African American church in the network to ask if congregants eligible for the vaccine who hadn’t signed up yet would be interested. Soon thereafter, those individuals were inoculated. That most likely wouldn’t have been possible if that nurse hadn’t spoken with congregants earlier to talk through their questions about the vaccine, Paulos said. “It was because of her; it’s not anything we’re doing.”
This illustrates the crucial role faith community nurses play in the wider medical ecosystem, Hinton said. “These are the people who are in the trenches doing the work, and they don’t really wave their flags for everybody to see.” Faith community nurses are the ones talking with people of faith day-in and day-out, offering essential medical advice that people trust, even when they don’t trust other institutions.
This is ministry on a deeper level, Hinton said. “From my perspective, a faith community nurse is the one carrying the hope.”
This article was made possible by gifts to the Mark Wingfield Fund for Interpretive Journalism.