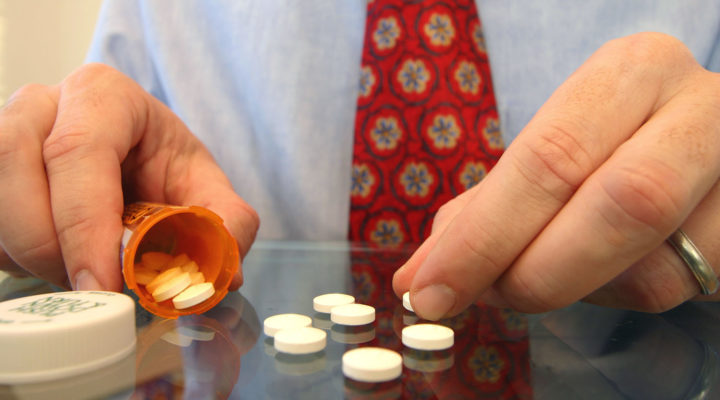
Opioid addiction can be so insidious and subtle it can turn almost anyone into an addict or enabler — even a minister.
Social worker Bryan Hatcher knows that from experience.
A North Carolina woman underwent medical procedures and for subsequent pain was prescribed an opioid, which includes familiar drugs like codeine, hydrocodone and Vicodin, among others.
Elderly and still recovering, the woman needed a monthly ride to see her physician. Her pastor — then Hatcher’s client — obliged. When the appointments became more frequent, the minister arranged for other church members to transport the 78-year-old grandmother to her growing list of doctor appointments.
It was when a surgeon refused to refill her pain medications that the pastor suspected something was wrong.
“Lo and behold, here he was helping her become an addict,” Hatcher said.
“This is a story that really catches me,” said Hatcher, a licensed clinical social worker and chief operating officer of CareNet of North Carolina, Inc., based in Winston-Salem, N.C. “Even she didn’t know what she was doing.”
Opioid deaths rising
The story illustrates how quietly yet steadily opioid addiction creeps up on its victims, and why many experts — including national health officials, ministers and domestic missionaries, health-care chaplains and law enforcement officers — describe the epidemic as among the worst on record.
Statistics from the Centers for Disease Control offer plenty of evidence. Currently, 91 Americans die every day from opioid addiction — many beginning with prescriptions for pain that evolve into heroin use. Annually, that adds up to more than 33,000 lives taken by the disease. The CDC also reports more than 500,000 deaths involving opioids from 2000 to 2015.
Heroin, which is considered the most addictive substance, is an opioid. Opioids are especially addictive because they flood receptors in the body, quickly killing pain but also causing high levels of tolerance and quick addiction, according to drugaddictiontreatment.com.
 Opioid addiction is considered “a more quiet epidemic” because so many of its victims are first exposed through prescriptions, says Georges Benjamin, executive director of American Public Health Association, headquartered in Washington D.C.
Opioid addiction is considered “a more quiet epidemic” because so many of its victims are first exposed through prescriptions, says Georges Benjamin, executive director of American Public Health Association, headquartered in Washington D.C.
“The initial exposure to opioids is primarily through a clinical route, though there also is a black-market route,” Benjamin said.
That distinguishes these cases of addiction from crack users, he added.
“The crack epidemic occurred very differently. It was associated with a lot of violence as drug dealers took over communities.”
Opioid addiction also has the distinction of practically no geographic or demographic limits. Its presence isn’t limited to urban areas.
“We are seeing more and more of this in rural America, among middle class folks,” Benjamin says.
But there are signs of hope, and some of it is credited to the work of religious groups and individuals in combating the epidemic.
Faith groups can deploy volunteers and resources and bring attitudes of compassion and emotional safety to bear for the victims of opioid addiction. Years of study and practical experience show faith can positively impact those suffering from all sorts of diseases, including addiction.
“Those who hold hope and have community, they do get better faster,” Hatcher says.
Generations of addicts
Scarlette Jasper is working to bring about just that kind of solace and healing, which is badly needed in the area where she ministers.
“It is a crisis and an epidemic here,” says Jasper, a Cooperative Baptist Fellowship field personnel serving a 10-county area near Lexington, Ky.
Much of what Jasper does in those impoverished, rural areas has nothing to do with addiction. She works with participants at a senior citizens center; runs financial literacy, nutrition and Bible study courses; and helps work against predatory lending.
But many of the other ministries she leads, such as food and clothing banks, are flooded by people afflicted, in one way or another, with opioid addiction.
It’s common for people she has helped on other issues, like poverty or domestic violence, to also be struggling with addiction directly or as a family member.
“One family I have worked with for 12 years, the parents have addictions and the adult children have addictions,” Jasper says. “In another family, two of the adult children have died from overdoses. One woman told me I would be preaching her funeral.”
With an acute shortage of drug-treatment facilities, the opioid epidemic is largely being treated through law enforcement, she says.
“Our jails are overrun with people with addiction. I minister to several people who are incarcerated now.”
When the state instituted a three-day maximum on prescriptions of addictive medications, addicts responded by turning to the streets.
“Now heroin is the big problem,” she says.
To add to the challenges, gun and domestic violence are on the rise in these communities.
All of this has led Jasper through a good bit of soul-searching on how to best respond as a minister. Her responses are evolving, but she feels her entire career has prepared her for this crisis.
“I am surrounded by people with mental health and addiction issues and I feel the Lord prepared me to work with those families. You wonder if you are helping but you keep at it because we have to be a voice for those who don’t have one.”
‘Plethora of churches’ responding
In Martinsville, Va., when overdoses and arrests began to spike at the beginning of the year, authorities there turned to churches. Police hoped religious groups could help on the front end of the epidemic.
“The faith community really stepped up,” Martinsville Police Chief Eddie Cassady said. “We made a pamphlet and they are taking it door to door warning of abuse, the effects of opioids, and how to get help.”
As a result of the team approach, the January spike in overdoses and violence has improved, he said.
Now, a church-bulletin insert is being designed that provides sobering statistics about opioid addiction. It also draws attention to the potency of the medications church goers may already have in their medicine cabinets.
“A lot of people don’t know they are being prescribed opioids,” Martinsville Assistant Chief Robert Fincher said.
Churches are ideal for the public awareness campaign and have been a big help to some addicts and family members who would rather approach their pastor than the police for help, Cassady said.
“That’s been another reason it’s been so important to have the faith community onboard.”
The awareness issue isn’t just for unwitting opioid users, but also for those in the community who have no idea there is an epidemic in the city, says Matthew Brown, pastor of St. Paul High Street Baptist Church in Martinsville.
“A lot of people, if they’re not out in the community as a police officer or in the medical field, they aren’t aware that we even have an opioid problem.”
The door-to-door campaign has been effective in alerting a larger segment of the community, he says.
It’s also brought together congregations across the denominational and racial spectrum. Many of them also are providing drop boxes where people can get rid of their unused medications.
“There is now a plethora of churches in this movement,” he says.
‘They are born addicted’
For chaplains, the fight against opioid addiction assumes an array of looks. One of those is in the emergency room, a setting that a Louisville television news crew recently observed during an assignment to follow an ER physician for a day.
They witnessed nine overdose cases coming through the ER doors in that one shift, said Matthew Eddlemen, a CBF-endorsed chaplain at Norton Audubon Hospital in Louisville.
“It’s almost daily that we have multiple overdoses come in,” he said. “It’s becoming unusual if we don’t have at least one.”
But that’s just scratching the surface for hospital chaplains.
Cases of addicted women giving birth are now commonplace, often overwhelming chaplains in delivery areas and neonatal intensive care units, because the infants are addicted, too.
“They are born dependent and they have to be weened off. They cry incessantly. It’s a very difficult thing for those babies,” says Kelley Woggon, director of Norton Healthcare’s Pastoral Care Department and a CBF-endorsed chaplain.
Staff working in those departments also need emotional and spiritual care after being constant eye-witnesses to the effect of opioids on infants, mothers and overdose victims. Seeing how family members are taken repeatedly through the wringer by their addicted loved ones also takes its toll on nurses, doctors and other medical workers.
Whether it’s among the staff or the families themselves, chaplains also struggle to address the desensitization that results from repetitive opioid addiction causes, Eddleman said.
“Some family members are fed up and want to cut off all contact, and then you have those family members who will go through hell and high water and say they will never give up, he says.”
Woggon recalls a father who had tried both sympathetic responses and tough love. “Nothing worked.”
Compounding the problem, some family members will supply the addict with drugs while they are hospitalized.
Though persons with an opioid addiction and their families respond differently, Eddleman and Woggon agree that all need a chaplain’s touch.
When they become aware of opioid addiction, congregations often want to know what to do about it.
Hatcher says he advises them to connect with other churches already providing relevant ministries. They can also host workshops on addiction.
But most of all, it’s about offering something churches should already be expert at: compassion.
“I would invite congregations to manage the stigma around all this by understanding that this disease is a process and how it works,” Hatcher says. “Faith must be about hope, not stigma and shame.”
Related stories:
Chronic pain sufferers feel forgotten in anti-opioid efforts
Former minster now ‘prisoner of pain,’ but art ‘transports’ him to place of purpose
Related opinion:
Opioid abuse is a tragedy, crack cocaine use is a crime. Why? | Russ Dean